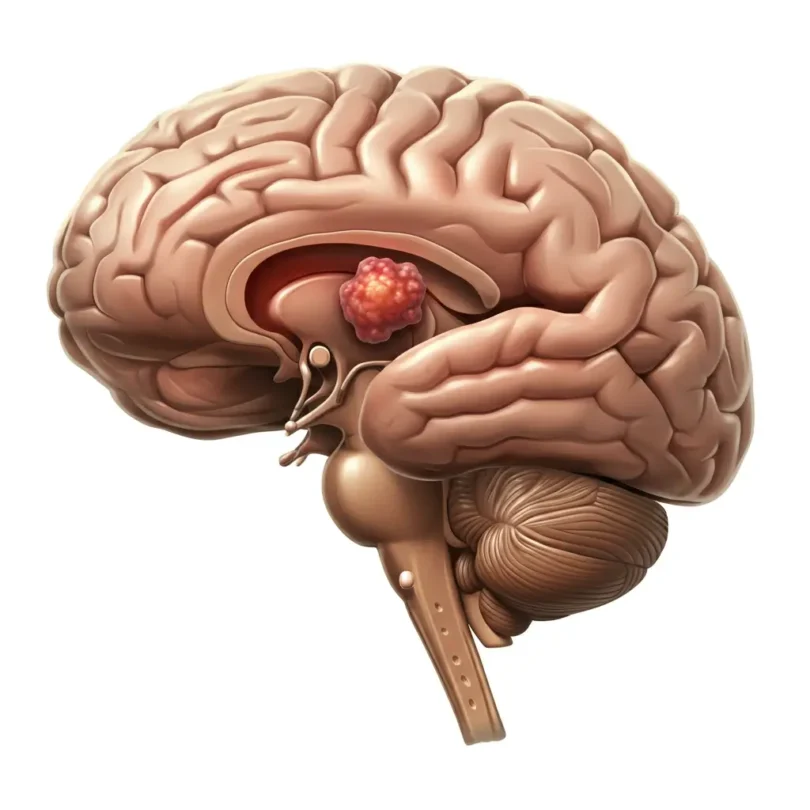
This is a rare benign tumor, most often occurring in children under 12 years. It represents less than 1% of all brain tumors. In children, the most frequent site of this tumor in the lateral ventricles. Plexuspapillome grow slowly inside the ventricles. They may block the flow of cerebrospinal fluid. This can cause hydrocephalus and increased the intracranial pressure. Papillomas of the choroid plexus are usually congenital neuroectodermal tumors, they make up about 1% of all tumors of the CNS. Most often they are sitting in the lateral ventricles, sometimes they are multiple, often sit in the 3rd ventricle or the cerebellopontine angle and in the cerebellomedullary cistern. Tumors of the 3rd ventricle often cause blurred vision and gait disturbances due to increased intracranial pressure as well as by direct pressure. Hydrocephalus arises by means of a transfer of CSF outflow routes (blockage of the foramen of Monro or Dubois Menschen aqueduct) and sometimes by obstruction of the outflow in the subarachnoid space. However, the tumor itself can also produce huge quantities of liquor. Most of these tumors are diagnosed in newborns and early childhood, indicating that they are innate.
Choroid Plexus Papilloma: Causes
Due to the relative rarity of choroid plexus papilloma, so far no statistical findings is present regarding possible causative factors for their emergence. The cancer research is not quite progressed in this area, because obviously there are no clear starting points.
This may be arise due to consequences of other diseases like Aicardi syndrome or the Li-Fraumeni syndrome. Aicardi syndrome is an X-linked genetic disease , which leads to undesirable developments in the brain. The autosomal dominant not gender typical, inherited Li-Fraumeni syndrome causes those affected to a high probability of multiple tumor illness at early age.
This approach also did not yield any verifiable findings. In conclusion it must be noted that still no scientific evidence is exists for the root causes of choroid plexus papilloma.
Choroid Plexus Papilloma: Symptoms
It will initially cause an increase in cranial pressure, lead to the unspecific symptoms like headache , nausea to vomiting , seizures and irritability. Especially in infants, where it is difficult to classify the non-specific symptoms properly, they remain hidden for long time and at an advanced stage it form a water head (hydrocephalus).
Due to the direct pressure that the choroid plexus papilloma exerts on the surrounding brain area also neuronal dysfunction may occur, cause the malfunction or failure of certain motor and / or sensory abilities.
Choroid Plexus Papilloma: Diagnosis
When nonspecific symptoms occur which are described above, which can be assigned to any particular disease occurrence, can suspected the presence of a neurological disease in the brain. During a Elektroencophalogramm (EEG) can help to detect early indications whether and where a brain tumor could arise while further clarification can be done by computed tomography ( CT ) and magnetic resonance imaging ( MRI ).
The focus of the diagnostics shifted from CT to MRI because the soft structures are displayed clearly by the MRI. An MRI can provide a good illustration of choroid plexus papilloma. The tissue of the tumor is emerging as a homogeneous mass with a cauliflower like structure. An analysis of the cerebrospinal fluid may help you to decide whether a nerve inflammation is present, which giving rise to the symptoms.
Last certainty that it is a benign or malignant tumor, provide by a biopsy followed by subtle investigation. Only the complete surgical removal of the tumor is an effective treatment.
Choroid Plexus Papilloma: Therapy and Treatment
Since there is no way to get rid of a choroid plexus papilloma by medications or other means. In case of a clear diagnosis, the complete surgical removal of the papilloma is the only effective treatment method available. Only in a few cases a significant relief of symptoms are obtained by an artificial drainage of cerebrospinal fluid, which reduces the intracranial pressure.
Specialized centers are fully capable to remove the tumor on microsurgical way or endoscopically as gently as possible. It is also aimed to enable the circulation of cerebrospinal fluid again by reopening possible outflows. During the operation, to increase the security the Neuronavigation and imaging techniques are used, enabling the constant monitoring of the operative procedure.
Among experts there is no consensus about whether postoperative continuation of treatment by radiation therapy is necessary and useful.
more general information about brain tumor: