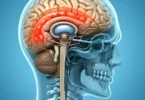
Astrocytomas
Astrocytic gliomas are the most common >>tumors of the brain with a share of 60% of all >>brain tumor.
There are two groups:
- The group of astrocytic >>tumors which are diffusely growing into the brain tissue consisting of
- Diffuse astrocytoma (WHO grade II)
- Anaplastic astrocytoma (WHO grade III)
- Glioblastoma (WHO grade IV).
- The group of astrocytic >>tumors with better delimited growth compared to the brain tissue, its main representatives the pilocytic astrocytoma (WHO grade I).
The >>tumors of the second group occur primarily in children and young adults. Tumor of second group grow relatively slowly and have a very low tendency to malignancy (<1%). A cure is possible, if tumor is full removed by operation. In contrast, the tumors of the first group occur primarily in adults, have a tendency to form malignant tumors and are characterized by a significantly worse prognosis.
Pilocytic Astrocytoma (WHO grade I)
It is a slow and circumscribed growing, well differentiated >>brain tumor with a favorable prognosis. Pilocytic astrocytomas are the most common >>brain tumors of childhood. About half of the >>tumors found in the anterior visual pathway and hypothalamic, about one-third in the cerebellum are Pilosytic tumor.
Diagnosis
The most important diagnostic method is the magnetic resonance imaging (MRI) of the skull. If this is not possible than computed tomography (CT) is used. The confirmation of the diagnosis is usually done by a surgical tissue removal . In the area of the optic nerve, this is associated with a risk of developing or increase of visual impairment.
Diffuse Astrocytoma (WHO grade II)
This is also a fine tissue well differentiated astrocytoma that grows slowly to the adjacent brain tissue without sharp boundary. Main location is the white matter of the cerebrum. Diffuse astrocytomas constitute 10-15% of astrocytic gliomas and tend to occur in young adults (peak age: 30 to 40 years). There is a tendency to move into an anaplastic astrocytoma or glioblastoma.
Diagnosis
The main diagnostic methods is magnetic resonance imaging (MRI) of the skull. If this is not possible, the computed tomography (CT) is used. The confirmation of the diagnosis is usually done by surgical removal of tissue.
Therapy
Due to the growth in a nearby tissues, complete surgical removal of the tumor is usually impossible. Extensive tumor resection is nevertheless seems useful. The conventional radiotherapy reduced the risk of relapse to a limited extent. It is often used only if tumor shows further growth after surgery. If the tumor shows further growth after surgery and radiotherapy, than chemotherapy may be used. In case of circumscribed >>tumors a local interstitial irradiation can also be used (brachytherapy).
Anaplastic Astrocytoma (WHO grade III)
These tumors show histological features of malignancy in favor of a rapid >>tumor growth. Anaplastic astrocytomas can either result from a pre-existing diffuse astrocytoma or newly formed astrosytoma. The peak age is between 35 and 45.
Diagnosis
The main diagnostic methods is magnetic resonance imaging (MRI) of the skull. If this is not possible, the computed tomography (CT) is used. The confirmation of the diagnosis is usually done by surgicaly removal of tissue.
Therapy
The therapy consists of surgery which is followed by radiation therapy or chemotherapy . In oligodendroglial >>tumors primarily chemotherapy also comes in question with PCV. The combination of radiotherapy and chemotherapy is controversial.
Glioblastomas (WHO grade IV)
Glioblastoma is the most common and most malignant astrocytic >>tumor. Glioblastomas account for more than half of all gliomas and preferably occur in the cerebrum in adults. The peak age is between 45 and 70 years. Most glioblastomas arise with short clinical history (primary glioblastomas). Glioblastomas that develop from a preexisting, diffuse or anaplastic astrocytoma are called secondary glioblastomas.
Diagnosis
The main diagnostic methods is magnetic resonance imaging (MRI) of the skull. If this is not possible, than computed tomography (CT) is used. The confirmation of the diagnosis is usually done by surgical removal of tissue . Certain laboratory tests (MGMT) should be carried out as a routine to decide whether chemotherapy should be performed or not. The importance of so-called molecular markers (such as MGMT) for therapy control is currently not yet been proven and should therefore only used in clinical trials for therapy selection.
Therapy
The therapy involves surgery which is followed by local radiotherapy. In addition, today chemotherapy with temozolomide is concomitantly to radiotherapy and then, usually, used for a further 6 months.